Veel mannen begrijpen niet wat hun prostaat doet en hoe deze hun leven kan beïnvloeden. De prostaat is een kleine klier ongeveer ter grootte van een walnoot, en ook met de vorm daarvan, die zich onder de hals van de blaas bevindt. De urinebuis loopt door het midden van uw prostaat, vanuit de blaas via de penis, en laat urine uit het lichaam wegvloeien.
Uw prostaat is een mannelijk voortplantingsorgaan. De belangrijkste functie van uw prostaat is om prostaatvocht te produceren. Het prostaatvocht is een alkalisch vocht dat tijdens de ejaculatie door de prostaatklier wordt uitgescheiden en dat deel uitmaakt van het zaadvocht.
Naarmate u ouder wordt, kan uw prostaat groter worden; gewoonlijk begint deze te groeien op de leeftijd van 40–50 jaar oud. Dit is een normaal deel van het ouder worden. Uiteindelijk kan deze groei leiden tot benigne prostaathyperplasie, beter bekend als BPH.
Benigne prostaathyperplasie, beter bekend als BPH of een vergrote prostaat, is een goedaardige vergroting van de prostaat en het omliggende weefsel.
BPH is een veelvoorkomende, aandoening bij mannen die wereldwijd meer dan 700 miljoen mannen treft1,2. Men vermoedt dat deze aandoening ontstaat als gevolg van hormonale veranderingen die optreden tijdens het ouder worden3.
In dit artikel leren we u alles wat u moet weten over BPH. Daarbij benadrukken we niet alleen wat het is en hoe het wordt gediagnosticeerd, maar ook hoe behandelingsmethoden zoals het UroLift-systeem snelle, effectieve verlichting kunnen bieden aan mannen die leven met symptomen van een vergrote prostaat4,5.
Om goed te begrijpen wat benigne prostaathyperplasie (BPH) inhoudt, moeten we eerst de prostaat nader bekijken.
De prostaat ligt bij mannen net onder de blaas en is een walnootvormige klier met drie hoofdfuncties6: hij speelt een rol bij de hormoonproductie, helpt bij het reguleren van de urinestroom en ejaculatieprocessen en produceert ook zaadvloeistof, een belangrijk bestanddeel van sperma.
Tijdens het leven van een man zal de prostaat twee belangrijke groeifasen doormaken. De eerste ontwikkeling vindt relatief vroeg in de puberteit plaats, wanneer de prostaat bijna twee keer zo groot wordt7. Vanaf ongeveer het midden van de twintiger jaren blijft de groei doorgaan gedurende de rest van het leven van een volwassen man, variërend van de grootte van een golfbal tot zo groot als een sinaasappel7.
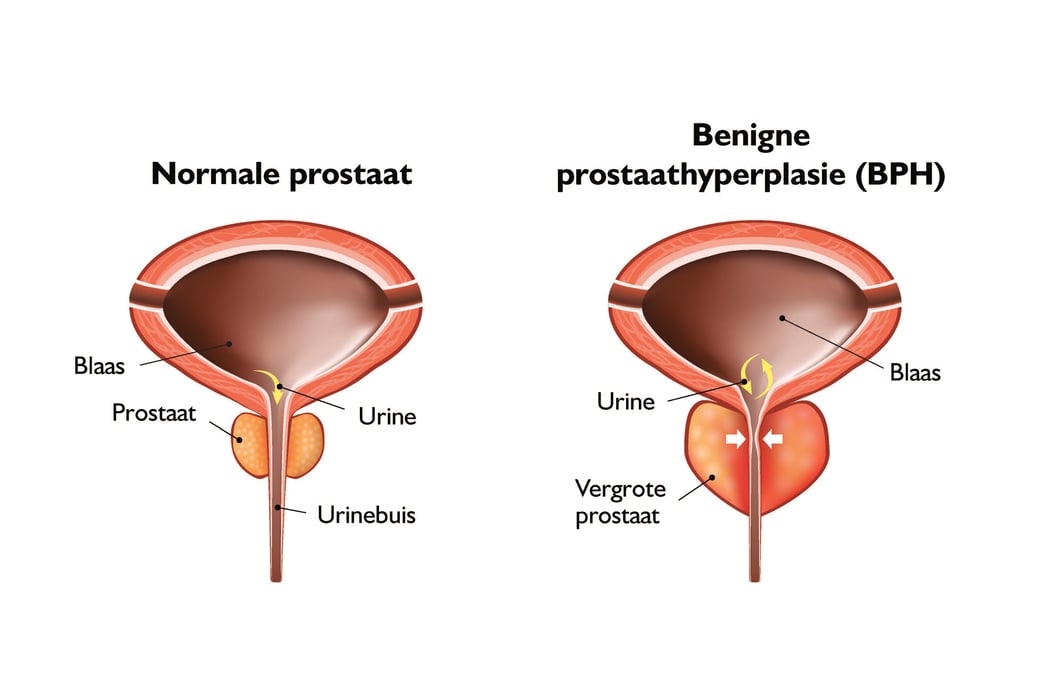
Symptomen van BPH ontstaan doordat de prostaat te groot wordt.
Wanneer dit gebeurt, kan de vergrote prostaat op de urethra (de buis waardoor urine de blaas kan verlaten) drukken en deze blokkeren. Hierdoor wordt de urethra afgekneld en wordt de blaaswand na verloop van tijd dikker. Dit kan vervolgens een breed scala aan hinderlijke urinewegklachten veroorzaken, zoals hieronder wordt toegelicht.
Een vergrote prostaat kan een aantal klachten veroorzaken die van invloed zijn op uw dagelijkse kwaliteit van leven. BPH is zelfs een van de tien meest voorkomende redenen waarom mannen de behoefte voelen om een uroloog te bezoeken8, zo heeft onderzoek uitgewezen dat 1 op de 4 mannen in zijn leven last kan krijgen van BPH9.
Deze symptomen hebben grotendeels invloed op het urinewegstelsel en omvatten vaak10,11:
Hoewel de exacte oorzaak van BPH nog relatief onbekend is, worden leeftijd en testiculaire factoren gezien als twee belangrijke elementen die hierbij een rol spelen12.
Mannen produceren gedurende hun leven testosteron en een kleine hoeveelheid oestrogeen. Naarmate ze ouder worden, begint de verhouding tussen de twee hormonen echter te verslechteren: de niveaus van actief testosteron beginnen te dalen, wat resulteert in een relatief hoger percentage oestrogeen in het bloed12.
Bepaalde studies gaan ervan uit dat deze relatieve toename van oestrogeenspiegels bepaalde groeibevorderende stoffen in de prostaat stimuleert, wat leidt tot BPH13.
Een andere theorie suggereert dat hoge niveaus van dihydrotestosteron (DHT) – een mannelijk hormoon dat een rol speelt bij de ontwikkeling van de prostaat – BPH veroorzaken. Onderzoekers hebben bijvoorbeeld aangetoond dat mannen die geen DHT produceren, ook geen BPH ontwikkelen12.
Wanneer we leeftijd als risicofactor beschouwen, spreken de onderstaande statistieken voor zich. Volgens een onderzoek gepubliceerd in het Journal of Urology1:
• Meer dan 40% van de mannen in de vijftig heeft BPH
• Meer dan 70% van de mannen in de zestig heeft BPH
• Meer dan 80% van de mannen in de zeventig heeft BPH
• Meer dan 90% van de mannen in de tachtig heeft BPH
Bepaalde andere risicofactoren kunnen het risico op het ontwikkelen van de aandoening ook vergroten. Dit zijn onder meer:
• Familiegeschiedenis – studies tonen aan dat mannen met een familiegeschiedenis van een vergrote prostaat een verhoogd risico hebben op het ontwikkelen van tekenen en symptomen die wijzen op BPH14.
• Etniciteit – onderzoek heeft uitgewezen dat het risico op BPH kan variëren, afhankelijk van de etnische groep. Zo hebben Afro-Amerikaanse mannen bijvoorbeeld ongeveer 50% minder kans om de diagnose BPH te krijgen dan blanke mannen15.
• Levensstijl – bepaalde factoren van de levensstijl, zoals roken, obesitas en gebrek aan lichaamsbeweging, worden allemaal geassocieerd met een verhoogd risico op BPH16.
Als u symptomen van BPH ervaart die uw algehele kwaliteit van leven beïnvloeden, hoeft u zich geen zorgen te maken: u bent niet de enige.
U kunt het beste eerst een afspraak maken met uw arts. Hoe dringend dat is, hangt echter grotendeels af van het soort symptomen dat u heeft.
Als BPH niet wordt behandeld, kan het op termijn een aanzienlijk risico vormen voor de blaasfunctie. Dit komt doordat de vergrote prostaat invloed kan hebben op de urethra, wat kan leiden tot lagere urineweg klachten, problemen met urineretentie of infecties vanwege het niet volledig legen van de blaas3.
Als u last krijgt van dergelijke symptomen of van andere ernstige problemen, zoals bloed in uw urine of problemen bij het plassen, dient u onmiddellijk een arts te raadplegen.
Tijdens het consult zal uw huisarts u een aantal vragen stellen over uw klachten en medische voorgeschiedenis. Daarna voert hij/zij een aantal tests uit om vast te stellen of uw prostaat vergroot is. Deze tests kunnen bestaan uit:
• Vragenlijst symptoomscore IPSS – opgesteld om te meten hoe ernstig uw urinewegsymptomen zijn door details vast te leggen over hoe vaak ze voorkomen
• Bloedonderzoek – om uw nierfunctie te beoordelen
• Bloedtest naar prostaatspecifiek antigeen (PSA) – om de hoeveelheid PSA in uw bloed te meten en te screenen op prostaatkanker
• Urineonderzoek – om te controleren op afwijkingen die kunnen wijzen op een onderliggende aandoening
• Rectaal toucher – uitgevoerd om de grootte en vorm van uw prostaatklier via uw rectum te voelen
Uw arts kan u doorverwijzen naar een uroloog voor nader onderzoek naar uw symptomen van BPH. Dit kan komen door terugkerende infecties, eerdere mislukte behandelingen, nierproblemen of een verhoogd PSA-niveau.
Wanneer u een specialist bezoekt, zal deze waarschijnlijk extra tests uitvoeren om de oorzaak van uw symptomen te bepalen. Dit kan het volgende omvatten:
• Urodynamisch onderzoek – om de zenuw- en spierfunctie, de druk rond en in de blaas, de stroomsnelheid en andere factoren te meten17
• Transrectale echografie – om gedetailleerde beelden van de prostaat te leveren die de grootte, vorm en structuur ervan benadrukken
• PSA-tests – om de hoeveelheid PSA in uw bloed te meten en te screenen op prostaatkanker
• Cystoscopie – om de urethra en de blaas te evalueren, waarbij ook wordt gekeken of de urethra door de prostaat wordt beïnvloedt12
Er zijn verscheidene opties om BPH te behandelen. Het vinden van de juiste behandeling hangt echter van diverse factoren af, zoals de ernst van uw klachten en de impact die ze hebben op uw dagelijks leven.
Samen met uw arts beslist u welke behandeling het beste bij uw situatie past.
Als u bijvoorbeeld alleen milde symptomen heeft, kunt u besluiten dat er helemaal geen behandeling nodig is. Moet u door uw symptomen vaker overdag en ’s nachts naar het toilet, dan kan een minimaal invasieve procedure zoals het UroLift-systeem worden aanbevolen.
Tijdens het eerste consult met uw arts kan hij/zij een meer afwachtende houding met u bespreken als uw BPH-symptomen mild tot matig zijn. Meestal houdt dit in dat u samen met uw arts uw prostaat in de gaten houdt, bijvoorbeeld aan de hand van een jaarlijks onderzoek, zonder dat er een actieve behandeling plaatsvindt.
Actief toezicht kan ook inhouden dat bepaalde veranderingen in de levensstijl worden doorgevoerd, zoals stoppen met roken, regelmatig bewegen en een gezond dieet volgen waarbij u vet- of suikerrijke en ook bewerkte voedingsmiddelen vermijdt16.
Bepaalde medicijnen kunnen worden voorgeschreven om de symptomen van BPH onder controle te houden en de urinestroom te verbeteren. Deze omvatten doorgaans18:
• Alfablokkers – ontspannen de spieren van de prostaat en helpen urinegerelateerde symptomen te verminderen. Ze kunnen echter ook bepaalde bijwerkingen veroorzaken, waaronder duizeligheid, vermoeidheid en ejaculatieproblemen.
• 5-alfa-reductaseremmers – verhogen de urinestroom en verminderen de productie van bepaalde mannelijke geslachtshormonen die bijdragen aan de groei van de prostaat. Het gevolg hiervan is dat de prostaat kleiner wordt, wat tot bijwerkingen als erectiestoornissen, ejaculatieproblemen en een verminderd libido kan leiden.
Voordat u medicijnen gaat gebruiken om uw BPH-symptomen te behandelen, is het belangrijk om eventuele zorgen die u heeft met uw zorgverlener te bespreken. Zij kunnen u alles vertellen over de mogelijke bijwerkingen van de verschillende soorten medicijnen. Ook kunnen ze ervoor zorgen dat uw behandelplan zo goed mogelijk aansluit bij uw persoonlijke omstandigheden.
Als u zich houdt aan het door uw arts voorgeschreven medicijngebruik, kunt u uw symptomen beter onder controle houden en kan dit uw algehele kwaliteit van leven verbeteren.
Als alternatieve benadering voor het innemen van medicijnen kan een minimaal invasieve operatie vaak dezelfde dag nog worden uitgevoerd, met een veel kortere hersteltijd dan de traditionele operatie.
Deze procedures zijn bedoeld om verlichting te bieden bij klachten aan de onderste urinewegen als gevolg van BPH. Ze worden normaal gesproken poliklinisch uitgevoerd onder plaatselijke verdoving.
Een minimaal invasieve aanpak die uw arts kan aanbevelen, is het UroLift-systeem.
Het wordt vaak uitgevoerd onder plaatselijke verdoving als poliklinische ingreep19 en werkt met behulp van kleine implantaten die vergroot prostaatweefsel optillen en vasthouden, weg van de urethra. Hierdoor verbetert de urinestroom en verminderen de bijbehorende symptomen.
Het UroLift-systeem is een bewezen aanpak voor patiënten die op zoek zijn naar een alternatief voor medicijnen of een ingrijpende operatie4. Het is ook de enige procedure voor een vergrote prostaat waarbij het prostaatweefsel niet hoeft te worden verhit, weggesneden, verwijderd of vernietigd5.
Bij meer ingrijpende operaties kan het nodig zijn om overtollig prostaatweefsel te verhitten, weg te snijden of te verwijderen. Typisch worden ze uitgevoerd onder algehele narcose, vereisen ze een ziekenhuisopname en kunnen ze het volgende omvatten:
• Transurethrale resectie van de prostaat (TURP)
• Transurethrale incisie van de prostaat (TUIP)
• Prostatectomie
• Laserchirurgie
U kunt ook contact opnemen met ons team als u nog vragen of opmerkingen heeft. Wij helpen u graag verder.
Veiligheidsverklaring
Het UroLift-systeem is geïndiceerd voor de behandeling van symptomen van een vergrote prostaat tot 100 cc bij mannen vanaf 50 jaar. Zoals bij elke medische procedure kunnen individuele resultaten variëren. De meeste bijwerkingen zijn tijdelijk en omvatten pijn en een branderig gevoel bij het plassen, bloed in de urine, bekkenpijn, sterke aandrang om te plassen en/of onvermogen om de aandrang te beheersen5. Zeldzame bijwerkingen, waaronder bloeding en infectie, kunnen ernstige gevolgen hebben en een medische ingreep vereisen. Overleg met uw arts om te bepalen of u in aanmerking komt.
Zie de gebruiksaanwijzing voor een volledige lijst van de indicaties, contra-indicaties, waarschuwingen en voorzorgsmaatregelen.
MCI-2023-0960
Broninformatie
Aangewezen voor de behandeling van symptomen van een vergrote prostaat tot 100 cc bij mannen van 45 jaar of ouder. Zoals bij elke medische ingreep kunnen de individuele resultaten variëren. De meest voorkomende bijwerkingen zijn tijdelijk en omvatten pijn of een branderig gevoel bij het plassen, bloed in de urine, bekkenpijn, dringende behoefte om te plassen en/of het onvermogen om de drang te beheersen (Roehrborn, J Urology 2013). Zeldzame bijwerkingen, waaronder bloedingen en infecties, kunnen ernstige gevolgen hebben en mogelijk een ingreep vereisen. Overleg met uw arts om te bepalen of u in aanmerking komt voor deze behandeling.
Teleflex, het Teleflex-logo, UroLift, het UroLift-logo, BPH Advisor, MyBPH Report en UroLift ATC zijn handelsmerken of geregistreerde handelsmerken van Teleflex Incorporated of haar dochterondernemingen in de Verenigde Staten en/of andere landen.
© 2026 Teleflex Inc. Alle rechten voorbehouden. | Gebruiksvoorwaarden | Internetprivacybeleid | Veiligheid van de patiënt | Indruk | Compliance